Clinical scenario 2: Penny
Teaching/Learning points:
- Cardiovascular assessment
- Physiological differences in children with shock
- Approach to resuscitation / fluids
- Blood on the floor… and four more (chest, abdomen, pelvis and long bone).
The emergency department receives an advanced warning from the ambulance service of a high-speed motor vehicle collision on the motorway nearby. At least three cars are involved and there have been a number of fatalities. Fire rescue services and a pre-hospital medical retrieval team are on the scene as a number of casualties are trapped and require extrication.
Your unit will be receiving Penny, a three year old female, who was found at the roadside some five metres from the main scene. It is thought she was ejected from one of the vehicles involved, in which two adult occupants died at the scene. She has been intubated at the scene due to reduced conscious level.
Vital signs are:
- Respiratory rate 25bpm (ventilated)
- Saturations 98% in 50% oxygen
- Heart rate 120bpm
- Blood Pressure 95/40.
She has multiple abrasions over her face and torso. ETA is 15 minutes...
The following nine questions refer to Penny’s clinical scenario.
|
Question 11 You are immediately considering the likelihood of Penny having significant traumatic injuries. Which factors in the pre-hospital alert DO NOT signify an increased risk of serious injury? |
|---|
| Three year old female |
| Ejected from vehicle |
| Fatalities in same vehicle |
| Abrasions over face and torso |
| Check answer |
ExplanationANSWER: Abrasions over face and torso. Penny is a paediatric patient in the pre-school age group, which makes her risk of poly-trauma and significant internal injury higher. In simple terms, her smaller size is likely to result in greater energy transfer in high-impact situations and wider transfer of forces to multiple body zones, i.e. combined head, chest, abdomen and pelvic injuries. Being ejected from a motor vehicle and the presence of fatalities in the same vehicle compartment are highly significant risk and prognostic factors for serious injury. |
|
Question 12 Penny arrives accompanied by a pre-hospital doctor and paramedic crew. She is immobilised on a spinal board with cervical collar in situ. She is intubated and mechanically ventilated. Her monitoring reads:
What is the best plan for an initial assessment of Penny? Identify the best order for the following steps by choosing from the answer options below:
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Disability or neurological status> Exposure> Airway with Cervical Spine control > Breathing> Circulation with haemorrhage control | ||||||||||
| Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Exposure> Disability or neurological status> Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control | ||||||||||
| Disability or neurological status> Exposure> Breathing> Airway with Cervical Spine control > Circulation with haemorrhage control | ||||||||||
| Check answer | ||||||||||
ExplanationAnswer: Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure In trauma, like resuscitation, an ABC approach is adopted for patient assessment and management (Airway, Breathing, Circulation, Disability, Exposure). In the case of trauma however, the mnemonic is modified to:
While in reality, assessment of these areas will run in parallel with a large team, rather than in series with one person, it is important to remember this sequence so as to identify the greatest threats to life first
|
|
Question 13 You commence your rapid primary survey with Penny’s airway, confirming correct endotracheal tube placement by direct laryngoscopy and end-tidal CO2 measurement. You maintain c-spine immobilisation as Penny is unconscious. On assessment of breathing, Penny’s chest wall is rising equally with good air entry bilaterally and good oxygen saturations. You therefore move on to cardiovascular assessment. Which of the following is NOT a priority in cardiovascular assessment in trauma? |
|---|
| Adequacy of circulation/Evidence of shock |
| Establish IV access |
| Evidence of bleeding/Haemorrhage control |
| Preventing hypertension |
| Check answer |
ExplanationAnswer: Preventing hypertension Assessing the adequacy of circulation, looking for evidence of shock: The commonest cause of shock in the context of trauma is hypovolaemic shock secondary to haemorrhage. Establishing good intravenous access: Necessary to support the circulation with volume and drugs. Looking for evidence of bleeding and controlling haemorrhage: The priorities at C are both to identify any obvious life-threatening injury to the circulatory system so it can be addressed as soon as possible, and to support the circulation where necessary to ensure adequate tissue delivery of oxygen and glucose, thus avoiding secondary injury. |
|
Question 14 Penny's heart rate is now 140bpm and Blood Pressure 95/40. Her radial pulses are palpable but thready compared to her carotid pulse. She is very cool peripherally and has mottled arms and legs. Her central capillary refill time is 4 seconds. Is Penny's circulation adequate? |
|---|
| Yes |
| No |
| Check answer |
ExplanationPenny is tachycardic, with evidence of poor central and peripheral perfusion. Additionally, Penny is in shock. Though more rigorous definitions of shock exist with strict criteria, a useful working definition of shock is: The failure of the cardiovascular system to maintain tissue perfusion. This is manifest at end-organ level by:
Some features are more rapidly identifiable than others, such as tachycardia/tachypnoea versus urine output, and some caution must be exercised when interpreting signs of potential shock:
|
|
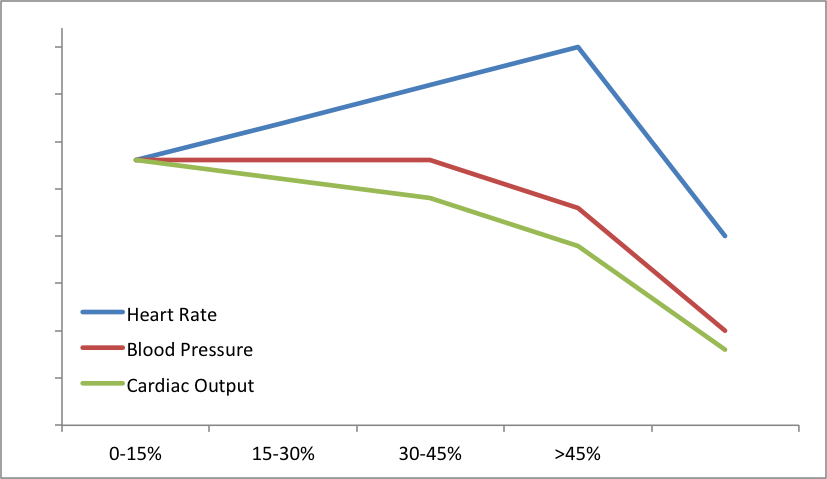
*Question 15 You establish Penny is in shock. On arrival, her heart rate was 120bpm and it has steadily risen during assessment, with evidence of poor perfusion. But, her blood pressure is stable. Unlike adults, hypotension is a late sign of shock in children, who generally have healthier cardiovascular systems. Children mount a more marked and sustained compensatory tachycardia to maintain blood pressure in the context of haemorrhage, before increasing systemic vascular resistance and blood pressure changes are seen.
The following graph illustrates:
Given the commonest cause of shock in the context of trauma is bleeding/blood loss (Hypovolaemic Shock), you suspect Penny has sustained significant haemorrhage. In the primary survey, which of the following sites is NOT rapidly assessed for evidence of haemorrhage/blood loss? Please note more than one answer may be correct. |
|---|
| Head |
| Chest |
| Abdomen |
| Pelvis |
| Limbs |
| The scene |
| Check answer |
ExplanationAnswer: Head. You can remember this as "Blood on the floor...and four more" (chest, abdomen, pelvis and long bones): Head: A closed head injury is unlikely to accommodate significant blood loss. If a head injured patient demonstrates signs suggestive of hypovolaemic shock, look elsewhere. There are caveats:
Chest: A large amount of blood can be accommodated in the chest and may be identified at B (assessment of breathing), either by obvious wounds/penetrations, or respiratory signs with distress, reduced air entry and a dull percussion note, and will require cautious drainage. Abdomen: A number of solid organs and large vessels in the abdomen are vulnerable either to blunt or penetrating injury and can bleed extensively. At younger ages, the liver, spleen and bladder are more abdominal and less protected by the ribcage and pelvis respectively, with greater risk of injury, including multi-organ injury. Pelvis: The pelvis contains a rich vascular supply, with the lower limb arteries and veins passing through it and a large sacral venous plexus. Fractures and shearing forces can cause significant bleeding, which can be contained, or tamponaded, within the closed bony pelvis. If however, pelvic fractures or injuries cause the pelvis to open outward (“open book” injuries), bleeding can continue catastrophically. Limbs: Children’s growing bones are very vascular; any open fracture can bleed significantly into the outside world. Certain larger long bones, such as the femur, if fractured and displaced, can accommodate a significant amount of occult blood loss into a potential space. The scene: Blood on the floor refers to obvious external haemorrhage, which can be immediately controlled with direct pressure. It is important to remember, however, that a patient may have left their blood behind at the scene. Never assume the paramedic crew will have noticed and told you. Also remember that 50% of every patient is on the other side, so inspect the patient’s back for bleeding or injury, ideally before it drips onto the floor. |
|
*Question 16 Which of the following trauma series x-rays is UNLIKELY to give information about the source of haemorrhage? |
|---|
| C-spine |
| Chest x-ray |
| Pelvic x-ray |
| Check answer |
ExplanationAnswer: C-spine. A significant haemothorax ought to be visible on chest x-ray as whiteout or haziness of the lung field. A fluid level is unlikely as the patient will be supine. Pelvic fractures, particularly an “open book”, are a potential source of life-threatening haemorrhage. Pelvic fractures are often multiple - think of the pelvic ring like a Lifesaver lolly: you can’t break it in just one place. |
|
Question 17* While establishing the cause of shock, it is necessary to resuscitate the patient by restoring and maintaining circulating volume. Penny has a small peripheral cannula in her hand through which her sedation is running. Ideally in trauma, large-bore, short length peripheral venous access is preferred (such as the brachial vein) for rapid administration of resuscitation fluids. When siting a cannula, blood is drawn for urgent crossmatch. If peripheral vascular access is difficult, there are a number of alternatives, including intraosseous access. You site a large bore cannula, send blood for urgent crossmatch and give Penny a bolus of warmed 0.9% sodium chloride. Current recommendations are to give up to 40mls/kg of crystalloid fluid (Normal Saline or Hartmann’s), in aliquots of either 10 or 20mls/kg, with frequent reassessment for response. In fluid resuscitation, patients often fall into three categories:
You reassess Penny repeatedly as you give fluids. Her chest remains clear and her abdomen seems full and firm. However, as she is intubated and sedated, it is difficult to ascertain tenderness: her pelvis feels intact, there are no evolving wounds or bruises and her long bones appear intact. Her heart rate continues to rise - it is now 160bpm - and her blood pressure is 80/50 after 40mls/kg of crystalloid fluids. By this stage, which of the following further resuscitation fluids should be given? |
|---|
| 0.9% sodium chloride, human albumin or glucose |
| Crossmatched blood, type-specific blood or O-negative blood |
| Human albumin |
| Type-specific blood |
| O-negative blood |
| Dextrose |
| Check answer |
ExplanationAnswer: The correct answer is Crossmatched blood, Type-specific blood or O-negative blood. Penny has received 40mls/kg of 0.9% sodium chloride, with no response. A child’s circulating blood volume is 60-80mls/kg. She has therefore potentially received 50% of her circulating volume in replacement boluses, with no response in heart rate or blood pressure. This is serious and implies massive haemorrhage somewhere. By this stage, if not earlier, we would aim to resuscitate with blood and blood products to replace losses like-for-like. The choice of blood depends slightly on the timeframe of need and availability:
It is important also to remember that clotting factors and platelets are lost or consumed in trauma. Most departments will have a “massive transfusion” protocol to ensure these blood products are given in addition to red cells. Current thinking, based on battlefield research, is cautious fluid resuscitation (10mls/kg boluses) to a low-acceptable blood pressure, rather than fluid overload, which potentially dislodges evolving clots. The thinking is that “the first clot (at the roadside) is the best clot.” |
|
Question 18 * You initiate emergency blood transfusion and call for assistance. Strongly suspecting abdominal bleeding, you request an urgent surgical consult. The surgeon agrees Penny has had significant haemorrhage and is extremely unwell. However, as Penny is so unstable, the surgeon is reluctant to take her directly to theatre to explore her abdomen in case this is not the source of bleeding. Which one of the following rapid tests might aid decision-making in this situation? |
|---|
| CT Abdomen with contrast (CTA) |
| Serum amylase |
| Abdominal X-ray (AXR) |
| Focussed Assessment Sonography in Trauma (FAST) |
| Diagnostic Peritoneal Lavage (DPL) |
| Check answer |
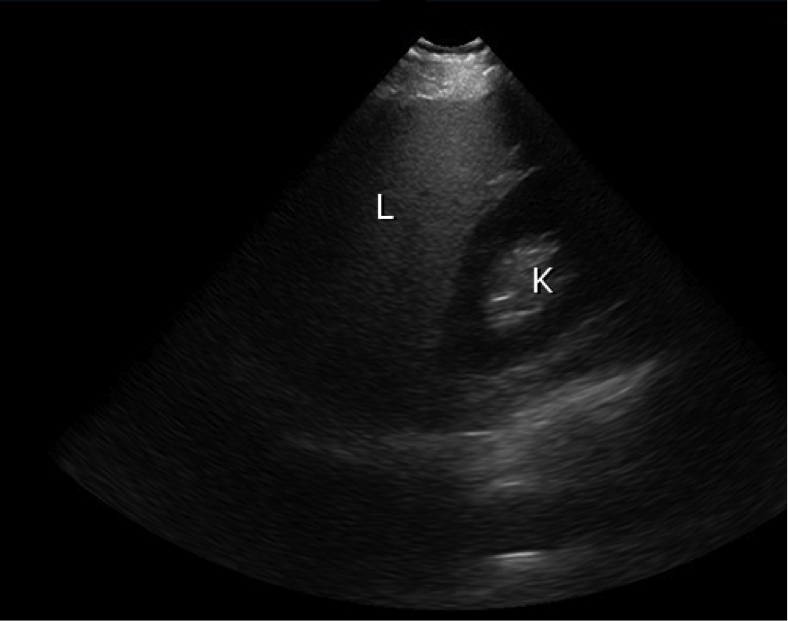
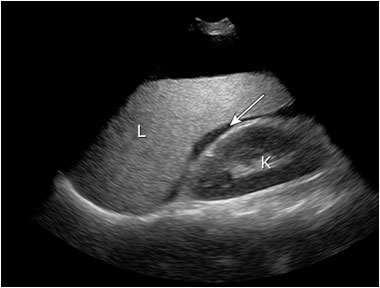
ExplanationA FAST scan is a focussed ultrasound that can be performed by a trained clinician in minutes. Views are obtained of four areas (hepatorenal, splenorenal, pelvis/bladder and xiphisternum) to identify the presence or absence of free fluid accumulating in the relevant potential spaces. The assumption is that in the context of trauma, this is blood. A negative FAST does not rule out bleeding, but a positive FAST effectively rules it in. Caution must be excercised, as FAST will not pick up retroperitoneal bleeds or contained intracapsular hepatosplenic bleeds. The accompanying two images were obtained as part of a FAST examination (not of Penny). The first shows normal juxtaposition of the liver and kidney without free fluid, while the second reveals free fluid surrounding the liver, as indicated by the arrow. Reference: UpToDate (www.uptodate.com)
A CT abdomen with double contrast is the gold standard in identifying abdominal or pelvic injuries. However, Penny’s clinical condition makes a trip to the scanner very risky as she is likely to deteriorate in the scanner, often called the 'Donut of Death' with good reason! There are few indications for a plain abdominal film; this is not one of them. |
|
*Question 19 You perform rapid FAST scan in resuscitation, confirming the presence of a significant amount of abdominal free fluid. The surgical team remain concerned about going straight to theatre. Which one of the following is the next best step in the definitive management of Penny? |
|---|
| CT Abdomen with contrast |
| PICU consult |
| Transfer to theatre for emergency exploratory laparotomy |
| Continue fluid resuscitation until stable |
| Commence inotropes |
| Check answer |
ExplanationAn unstable trauma patient, unresponsive to fluid resuscitation and with a positive FAST scan needs to be transferred to theatre for laparotomy. This can often be a difficult decision to make. However, Penny is unlikely to get any more “stable” without identification and repair of her bleeding. PICU will have nothing to add. Further fluids should continue but not delay transfer and inotropes alone are unlikely to help if the pipes are empty. Penny needs to be transferred to theatre to “stop the tap”. |