Clinical scenario 1: James
Teaching/learning points:
- Initial ABC approach to trauma patient
- Recognition of life-threatening injury and resuscitation priorities
You receive a pre-hospital alert from paramedics regarding James, a four year-old boy who ran away from his mother onto the road, where he was hit by a van at approximately 50kph. He hit the windscreen and was thrown approximately 7 metres. He was unconscious at the scene and not moving spontaneously. The paramedic crew on the scene report him to be unconscious but breathing, with a respiratory rate of 30/min, heart rate 120bpm, multiple abrasions and bruises. ETA 10 minutes.
The following 12 questions refer to James' clinical scenario.
|
Question 01 What is the best plan for an initial assessment of James? Identify the best order for the following steps by choosing from the answer options below:
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Disability or neurological status> Exposure> Airway with Cervical Spine control > Breathing> Circulation with haemorrhage control | ||||||||||
| Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Exposure> Disability or neurological status> Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control | ||||||||||
| Disability or neurological status> Exposure> Breathing> Airway with Cervical Spine control > Circulation with haemorrhage control | ||||||||||
| Check answer | ||||||||||
ExplanationAnswer: Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure In trauma, like resuscitation, an ABC approach is adopted for patient assessment and management (Airway, Breathing, Circulation, Disability, Exposure). In the case of trauma however, the mnemonic is modified to:
While in reality, assessment of these areas will run in parallel with a large team, rather than in series with one person, it is important to remember this sequence so as to identify the greatest threats to life first
|
James arrives with the paramedic crew, secured on a long spinal board with a hard cervical collar and sandbags fitted. He is unresponsive, making snoring/gurgling inspiratory noises. There is blood and dirt over his face and he has multiple bruises/abrasions. His breathing is laboured.
|
Question 02 Following the initial assessment, which one of the following would be the best first intervention? |
|---|
| Head tilt and chin lift |
| Inspect the airway and perform jaw thrust |
| Insert a suction catheter into the mouth |
| Check answer |
ExplanationPerforming a head tilt and chin lift in this context would be contraindicated, and risks worsening any underlying c-spine injury. Blindly inserting a suction catheter into the mouth risks causing trauma/bleeding, and potentially forcing a foreign body further down. Visually inspecting the airway allows safe suctioning of any visible obstructions i.e. blood/vomit/teeth. With the patient immobilised in a collar, a jaw thrust is the only safe manoeuvre to open the airway by lifting the tongue forwards. |
|
Question 03 Is the following statement true or false? Children have relatively larger heads with proportionally small jaws. |
|---|
| True |
| False |
| Check answer |
ExplanationThis is particularly true in younger children. This makes the head a greater target in trauma and accounts for head injury being far more common. A comparatively smaller jaw, shorter airway and higher, more anterior larynx require consideration when managing the paediatric airway as the tongue has a greater tendency to obstruct and different instruments are needed for airway management. When small children are laid flat, their larger occiputs will naturally cause the neck to flex, requiring additional attention when protecting the cervical spine and airway. |
|
Question 04 Following the intervention, James’ breathing improves and the noises cease. Before moving on in your assessment, which one of the following adjuncts would be beneficial? |
|---|
| Insertion of a nasogastric tube |
| Removal of jewellery/earrings |
| Administration of high-flow oxygen |
| Clean wounds before mother arrives |
| Check answer |
ExplanationAll major trauma patients benefit from high flow oxygen via non-rebreath mask. The routine administration makes it less likely to be forgotten in those who really need it. |
|
Question 05* You move on to assess James’ breathing. When rapidly assessing a child’s breathing, we think in terms of effort, efficacy and effects. Which grouping of the signs and observations below would best indicate effort? |
|---|
| Respiratory Rate, Chest wall expansion, Subcostal/Intercostal Recession, Tracheal Tug |
| Oxygen Saturations and Skin Colour, Heart Rate, and Conscious level |
| Air entry (Equal bilateral), and Added sounds |
| Check answer |
ExplanationEffort is best indicated by:
|
|
Question 06* Which grouping of the signs and observations below would best indicate efficacy? |
|---|
| Respiratory Rate, Chest wall expansion, Subcostal/Intercostal Recession, Tracheal Tug |
| Oxygen Saturations and Skin Colour, Heart Rate, and Conscious level |
| Air entry (Equal bilateral) and Added sounds |
| Check answer |
ExplanationEfficacy is best indicated by:
|
|
Question 07* Which grouping of the signs and observations below would best indicate effects? |
|---|
| Respiratory Rate, Chest wall expansion, Subcostal/Intercostal Recession, Tracheal Tug |
| Oxygen Saturations and Skin Colour, Heart Rate, and Conscious level |
| Air entry (Equal bilateral), and Added sounds |
| Check answer |
ExplanationEffects is best indicated by:
|
|
Question 08 * Currently James is breathing at a rate of 50 breaths per minute, with his right side apparently moving more than his left. There are a few bruises over the anterior left chest but no obvious wounds or deformities. There is poor air entry on the left side compared to the right. Oxygen saturations are 98% in high flow oxygen (88% in air), heart rate 120bpm and conscious level remains decreased. At this stage, there is suggestion of a serious breathing problem to address before moving on. Which one of the following pieces of additional information would be helpful in deciding the next steps? |
|---|
| Tactile vocal fremitus |
| Arterial blood gases |
| Percussion note |
| Peak expiratory flow |
| Check answer |
ExplanationIn the assessment of breathing in the injured child, a number of the main life-threatening injuries reside in the chest. In the context of reduced air entry on one side, percussion note will help differentiate between pneumothorax (hyper resonant) and haemothorax (dull) and guide further lifesaving treatment. This can be challenging in the noisy resuscitation room. The 'Lethal Six' are:
|
|
Question 09 * Is the following statement true or false: Children have weaker ribs that are more prone to fracture. |
|---|
| True |
| False |
| Check answer |
ExplanationChildren do have softer ribs, but not weaker. They are much more pliable and less likely to fracture. Therefore, they more readily transfer energy to the viscera, with a much higher incidence of injuries such as pulmonary contusion in the absence of chest wall damage or rib fracture. The presence of rib fractures indicates significant force and requires a high Menu of suspicion for chest organ injury. |
|
Question 10 * James has increased work of breathing and hypoxia in the context of reduced left sided air entry, reduced left chest wall movement, and a hyperresonant percussion note. Which one of the following is this clinically suspicious of? |
|---|
| Massive haemothorax |
| Great vessel injury |
| Pneumothorax |
| Diaphragmatic rupture |
| Check answer |
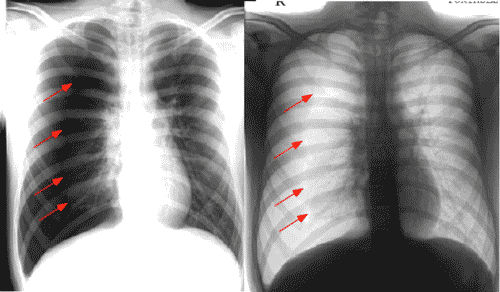
ExplanationThese clinical features are suggestive of the presence of air in the chest, between the lung and chest wall. Here is a radiograph of a spontaneous pneumothorax in a child. Tap or click image for full size. The left-hand image represents a conventional radiograph. A large right pneumothorax is demonstrated. The visceral pleural line is marked by red arrows. The lack of vascular and pulmonary markings in the periphery should be noted. The right-hand image represents the negative image of the film on the left. The pneumothorax is more clearly seen in this view. Reference: UpToDate (www.uptodate.com) |
|
Question 11 * Pneumothorax is potentially life-threatening if it is a tension pneumothorax. In this case, you need to consider other signs. Which one of the following is NOT a sign you need to consider for tension pneumothorax? |
|---|
| Hypoxia |
| Tachycardia |
| Hypotension |
| Distended neck veins |
| Hypoglycaemia |
| Tracheal deviation |
| Check answer |
ExplanationAnswer: Hypoglycaemia. Respiratory distress, hypoxia, tachycardia and low blood pressure, with visible distended neck veins and tracheal deviation in a trauma patient with decreased air entry and hyper-resonant percussion note, are highly suggestive of tension pneumothorax, which is rapidly life-threatening. Note tracheal deviation and distended neck veins can be difficult to spot when a child is wearing a c-spine collar and in shock. |
|
Question 12* Which one of the following is the most appropriate intervention at this stage? |
|---|
| Chest x-ray to confirm suspicion |
| Insertion of surgical chest drain |
| Immediate needle decompression |
| Intubation |
| Check answer |
ExplanationA true tension pneumothorax is very poorly tolerated and rapidly decompensates. Due to a ball-valve effect, air leaks between the pleura during inspiration but remains trapped. The pneumothorax enlarges, causing mass-effect on the mediastinum, ultimately impairing venous return to the heart. Hence, distended neck veins and cardiac output. The correct emergency procedure is needle decompression by inserting the largest possible IV cannula vertically through the chest wall into the pleural space at the mid-clavicular line of the second intercostal space. This releases the tension, converting the tension pneumothorax into a simple pneumothorax. A chest x-ray would confirm the diagnosis but the child could die waiting. Insertion of a surgical chest drain will be necessary in due course to fully treat the pneumothorax, but again, could prove too time-consuming to immediately relieve the tension. Intubation and positive-pressure ventilation will make things worse. If necessary, a chest tube is required to avoid creating a tension pneumothorax from a simple one. Following the needle decompression, James is prepared for chest drain insertion and his circulation is assessed. |