Clinical scenario 1: Johnny
Teaching/Learning points:
- Rapid neurological assessment
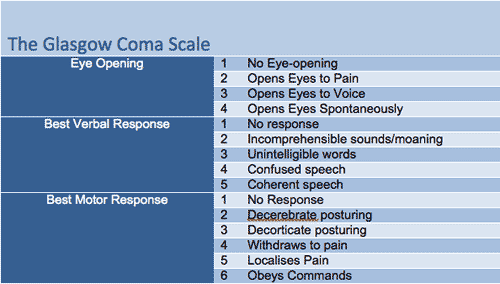
- GCS including AVPU and Modified GCS
- Prevention of secondary insult
Jonny is a 10 year old boy. He is en-route to the emergency department via ambulance following a fall from his bike. Paramedics have called ahead, stating Jonny was riding downhill and hit the side of a parked car at the bottom. He was thrown over the car, landing on the street. He was not wearing a helmet and was apparently knocked unconscious.
He is described as semi-conscious, breathing at a rate of 18/min, sats 98% in air, heart rate 90pbm. He has a large swelling to the right side of his head, and no other obvious injuries. Their ETA is 15 minutes.
The following ten questions refer to Jonny’s clinical scenario.
|
Question 01 What is the best plan for an initial assessment of Jonny? Identify the best order for the following steps by choosing from the answer options below:
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Disability or neurological status> Exposure> Airway with Cervical Spine control > Breathing> Circulation with haemorrhage control | ||||||||||
| Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure | ||||||||||
| Exposure> Disability or neurological status> Breathing> Airway with Cervical Spine control> Circulation with haemorrhage control | ||||||||||
| Disability or neurological status> Exposure> Breathing> Airway with Cervical Spine control > Circulation with haemorrhage control | ||||||||||
| Check answer | ||||||||||
ExplanationAnswer: Airway with Cervical Spine control> Breathing> Circulation with haemorrhage control> Disability or neurological status> Exposure In trauma, like resuscitation, an ABC approach is adopted for patient assessment and management (Airway, Breathing, Circulation, Disability, Exposure). In the case of trauma however, the mnemonic is modified to:
While in reality, assessment of these areas will run in parallel with a large team, rather than in series with one person, it is important to remember this sequence so as to identify the greatest threats to life first
|
|
Question 03 Happy with ABC, you move on to rapidly assess D. Rapid clinical assessment of neurologic status consists of establishing conscious level and pupillary responses. Which one of the following is a useful initial approach to assess Jonny’s neurologic status? |
|---|
| Ask 'Are you alright?' |
| Shake the patient by the head |
| Check deep tendon reflexes |
| Apply a painful stimulus |
| Check answer |
ExplanationA useful clinical approach for rapid assessment is simply to ask your patient “are you alright?” This sounds obvious, but the patient who responds is telling you:
A GCS or AVPU score can be calculated thereafter based on the patient’s response to simple questions. The patient who does not respond appropriately (or at all) can then be evaluated with increasing levels of stimulus, ie voice, touch, pain. |
|
Question 04 In the emergency department, Jonny appears unconscious, he opens his eyes briefly to a painful stimulus and moans incomprehensibly. He withdraws his limbs when a painful stimulus is applied. Which one of the following is Jonny’s current GCS? |
|---|
| 12 |
| 4 |
| 8 |
| 10 |
| 14 |
| Check answer |
Explanation
Total = 8 It would also be reasonable to say that Jonny is a P on the AVPU scale. (A GCS of 8 is felt to correlate roughly with P on the AVPU scale). A GCS of 8 is of particular importance as it thought that a patient’s protective airway reflexes become impaired at around this level of decreased consciousness |
|
Question 05 On further questioning of the paramedic crew, they report that when they first arrived on the scene, eyewitnesses said Jonny had been unconscious for 5-10 minutes. When they assessed him, he would open his eyes to verbal stimulus, responding to questions with unintelligible and/or meaningless words, but he would localise painful stimulus by pushing their hands away. Which one of the following was Jonny’s GCS at the scene? |
|---|
| 3 |
| 5 |
| 7 |
| 9 |
| 11 |
| Check answer |
Explanation
Total = 11 This is useful information, as there is evidence that initial GCS at scene, particularly the motor component, correlates with ultimate/long-term prognosis. The neurosurgical team will want to know this. |
|
Question 06 This information suggests Jonny's conscious level is deteriorating. As part of your neurological assessment, you review Jonny’s pupils:
Which one of the following is suggested by these clinical findings? | |||||||
|---|---|---|---|---|---|---|---|
| A lazy eye | |||||||
| Migraine | |||||||
| Eye trauma | |||||||
| Raised intracranial pressure | |||||||
| Shock | |||||||
| Check answer | |||||||
ExplanationIn the context of head injury, unequal or unreactive pupils are a major red-flag sign of raised ICP and can progress rapidly to coning and death. To understand the mechanism of this, think of the skull as a closed box:
Inside the box sits the brain, bathed in cerebral spinal fluid (CSF) and perfused by blood in arteries and veins.
In closed head injury, bleeding occurs, which occupies space in the closed box and squashes the other components in the box because the box can’t expand. The body can cope with this to an extent via the ventricular system but eventually will reach a point where either circulation to the brain is compromised or the brain itself is squeezed irrevocably. This is manifest clinically with a decrease in conscious level and pupillary abnormalities. Ultimately pressure can force the brain to herniate at the tentorium or the brainstem (coning), leading to loss of vital functions and death. The so-called Cushing’s Triad of bradycardia, hypertension and abnormal breathing, a manifestation of this brainstem pressure, is a very late and grave sign in children. Children are also peculiarly more prone to cerebral oedema in head injury than adults. |
|
Question 07 There is concern that Jonny has a significant closed head injury, with deteriorating conscious level and pupillary abnormalities suggestive of rising intracranial pressure. His cardiorespiratory status at this stage is satisfactory and suggestive of an isolated head injury. You notify the neurosurgical team of the situation. From the following answer options, choose the best set of three management steps for Jonny.
|
|---|
| B, C, D |
| A, C, D |
| A, B, D |
| A, B, C |
| C, D, E |
| Check answer |
ExplanationA, B, C - Intubation and Osmotic Diuretics In this context of head injury with deteriorating conscious level, one needs to consider the safety of the patient’s airway (due to loss of protective reflexes and risk of aspiration rather than direct injury) and breathing (hypoventilation secondary to coma). Therefore it is common to pre-emptively secure the patient’s airway by Rapid Sequence Intubation. However, care must be taken when choosing induction agents as some can directly raise ICP (Ketamine) and others are particularly vasoactive in cardiovascular instability (Propofol). Additionally, care must be taken when performing laryngoscopy and tracheal intubation as both can stimulate a rise in ICP. 20% Mannitol, and more recently, hypertonic saline (3%), are given in the setting of acutely rising ICP. Both act by osmotic diuresis to transiently assist decompression, buying time for preparation of definitive management. Our plan at this stage is to:
Urgent neuro-imaging (most often CT) will assist the neurosurgical team in planning how to proceed by identifying the site, nature and extent of the injury. In trauma, and particularly head trauma, the concept of optimisation and prevention of secondary injury features alongside resuscitation. The mortality and morbidity associated with major trauma is often thought of as trimodal, with death and disability occurring:
|
|
Question 08* Jonny is now intubated, sedated and ventilated in the resus room. Which of the following aspects of his physiology should be monitored to limit the development of secondary brain injury? |
|---|
| Blood glucose |
| Blood pressure |
| Head position |
| Temperature |
| CO2 |
| Sodium |
| Oxygen |
| All of the above |
| Check answer |
ExplanationAll of the above. These are so-called Neuroprotective measures. Blood Glucose: Neurones are metabolically very active and dependent on glucose for fuel, with no alternate fuel source. Therefore, sustained hypoglycaemia is poorly tolerated generally, let alone in the setting of an injured brain. Sustained hypoglycaemia leads to global brain injury. Equally, sustained hyperglycaemia in critical care patients is associated with adverse outcome. Blood pressure: Maintaining a good blood pressure in head trauma is critical to maintaining cerebral perfusion pressure (CPP). CPP is the pressure difference between ICP and Mean Arterial Blood Pressure. It is this pressure difference that supplies the brain with oxygenated blood. As ICP rises or BP falls in head injury, CPP drops proportionally, ultimately compromising cerebral blood flow. Head Position: Positioning the patient with a 10-15 degree head-up tilt helps to encourage cerebral venous drainage. Temperature: A lot of research is looking into the role of active cooling in various contexts of cerebral insult to decrease cerebral oxygen demand, metabolic rate and inhibit damaging inflammatory responses. While in the context of head trauma the role of active cooling is not fully established, it is accepted that hyperthermia is best avoided as it causes the reverse of the noted cooling effects. CO2: Hypercapnia causes cerebral vascular dilatation, which can worsen bleeding and increase ICP. Conversely, hypocapnia causes cerebral vasoconstriction, impairing cerebral blood flow. Neither situation is ideal, therefore ventilation strategies aim to maintain CO2 in the normal range with careful monitoring. Sodium: Maintaining electrolyte homeostasis, particularly sodium, is of importance in preventing fluid shift, cerebral oedema and cell death. Hypertonic saline is often employed in the emergency setting of raised ICP, but maintaining sodium in the normal range to avoid subtle fluid shift is also important. Oxygen: The brain is metabolically active and dependant on aerobic respiration. The injured brain even more so. Therefore, good oxygenation is essential to prevent secondary brain injury. |
|
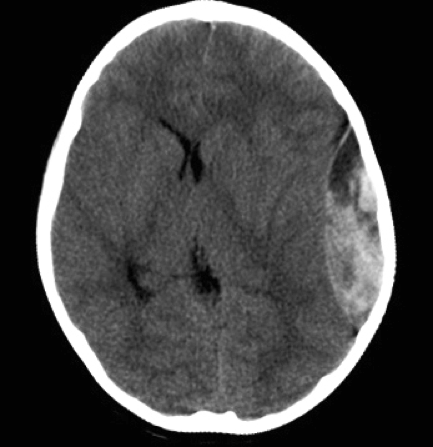
Question 09* After reassessing Jonny's ABCDEs and ensuring he is as stable as possible, you assist in transferring him for a CT scan. The scan is performed rapidly, producing the accompanying image.
Reference: UpToDate Which one of the following is shown in the CT scan? |
|---|
| Frontal skull fracture |
| Right subdural haematoma |
| Subarachnoid haemorrhage |
| Right extradural haematoma |
| Left extradural haematoma |
| Check answer |
ExplanationA left extradural haematoma is shown, with its classical “lenticular” appearance. The haematoma is causing some midline shift, with deformation of the ventricles, giving them an unequal appearance. The dark swirls in the haematoma represent rapid arterial bleeding. |
|
Question 10 On recognition of his extradural haematoma, Jonny is transferred urgently to theatre, where he undergoes neurosurgical intervention to evacuate the haematoma, before transfer to PICU. In contrast to adult injury patterns, children have a higher incidence of isolated head injury in major trauma. Traumatic brain injury represents a huge proportion, not only of mortality, but also morbidity in paediatric trauma as survivors with long-term neurological impairments present significant social, emotional and financial costs to their families and local healthcare services. Bicycle crashes are the second leading cause of traumatic brain injury in children. Which one of the following preventive measure could have significantly influenced this case? |
|---|
| Reducing the speed limit on residential streets |
| Greater provision of cycle paths |
| Wearing a helmet |
| Wearing high-visibility clothing |
| Mandatory cycling proficiency testing |
| Check answer |
ExplanationWearing a cycling helmet is the only preventive intervention to have been shown to reduce the incidence and severity of traumatic brain injury in bike accidents. |