Clinical scenario 3: Jenna
Jenna, a four month old girl, presents with a one day history of fever, fussiness and poor feeding. She is irritable and difficult to console but is breathing comfortably on her own and maintaining a good airway. She does not like to be moved. Vital signs:
RR 36min, HR 120/min, BP 90/58 mmHg.
Temperature 39.2° C and SaO2 98% in room air.
Her fontanelle appears full and her neck appears slightly stiff. CRT < 2 seconds.
The following seven questions refer to Jenna’s clinical scenario.
|
Question 11 Which ONE of the following is the most likely diagnosis? |
|---|
| URTI |
| Meningitis |
| UTI |
| Encephalitis |
| Not possible to determine |
| Check answer |
ExplanationThis child has features suggestive of meningitis, given her irritability and full fontanelle. The diagnosis of meningitis may be more difficult in the very young as history and examinations can be non-specific. Note that young infants with meningitis may not have neck stiffness. Features include:
A high menu of suspicion for meningitis must exist in sick, febrile or hypothermic newborns, with or without the above features. |
|
Question 12 What is your approach to her management? Place the appropriate options in the order in which you would perform them, but choose only those that are necessary for Jenna. A) Lumbar puncture and bloods for FBC, UEC, CRP, Blood culture |
|---|
| B, A, C |
| B, C, E |
| B, C, D |
| E, B, A |
| C, D, A |
| Check answer |
ExplanationB, A, C – Attend to airway, breathing and circulation, Lumbar puncture and bloods for FBC, UEC, CRP, Blood culture, and dexamethasone. Then commence antibiotics.
For children over three months, there is evidence that early administration of dexamethasone before commencement of antibiotics has beneficial effects on hearing impairment in HIB and non-HIB meningitis. |
|
Question 13 A lumbar puncture is performed. Place the following five steps in the correct order for performing a lumbar puncture. A) Positioning of child |
|---|
| E, A ,C, B, D |
| A ,C, B, D, E |
| C, B, D, E, A |
| B, D, E, A ,C |
| D, E, A ,C, B |
| Check answer |
ExplanationD-E-A-C-B Parental consent, local anesthetic patch, positioning of child, clean area, and insertion of needle and collection of fluid. It is important to gain consent for an LP. A full explanation of the procedure should be given, including a fact sheet. Local anaesthetic cream is usually placed on the lower back unless the LP is being performed as a matter of extreme urgency. Injection of local anaesthetic is also used but may obscure landmarks. In many units, inhaled nitrous oxide or a mild sedative such as oral midazolam may be given to an older child. Oral sucrose should be considered in a neonate. The child needs to be positioned on their side with their legs curled up under their chin. A nurse is required to assist with positioning and to keep the child still. An LP is a sterile procedure. The skin over the lower back is cleaned with iodine or chlorhexidine. Sterile drapes are placed around the site. The needle is inserted into the spinal space between L3-L4 or L4-L5. This is located by palpating the posterior-superior iliac crest and drawing an imaginary line between the two crests that intersect with L4. The needle is inserted with the bevel facing up and aiming cephalad towards the umbilicus, advancing slowly. Since penetration of the dura is not always obvious. The stylet can be removed from time to time during insertion to look for CSF. A “pop” is sometimes heard as the needle enters the subarachnoid space. CSF should be collected in 3-4 separate numbered tubes with approximately ten drops in each tube. The stylet should then be replaced and the needle removed. A dressing should be placed over the site. As with all procedures in paediatrics it is important to be able to describe the procedure in lay terms for the parents. Reference: |
|
Question 14 Which of the following are the TWO most likely complications of an LP? |
|---|
| Introduction of infection and traumatic tap |
| Traumatic tap and unsuccessful procedure |
| CSF leak, and nerve involvement - paralysis |
| Unsuccessful procedure and introduction of infection |
| Nerve involvement - paralysis and CSF leak |
| Check answer |
ExplanationAll of these are potential complications. By far the most common is a traumatic e.g: blood stained tap (making immediate interpretation more difficult) and an unsuccessful procedure. Other complications include dermoid from introduction of skin tissue during procedure, headache (hard to determine at this age) and coning (less risk with open anterior fontanelle) |
Clinical scenario: Jenna continued
The preliminary CSF results show:
- CSF glucose 4mmol/L (3-5)
- CSF protein 0.99g/L (<0.4)
- Cell count (x10’6/L)
- polymorphs 1300
- lymphocytes 60
- red cells 2
- Cell count (x10’6/L) red cells
- Gram stain – no organisms seen
|
Question 15 Which ONE of the following is the most likely cause of the meningitis demonstrated by this CSF result? |
|---|
| Viral |
| Bacterial |
| Tuberculosis |
| Traumatic tap |
| Fungal |
| Check answer |
ExplanationThe presence of polymorphonuclear (PMN) cells should always be assumed to be abnormal and usually suggests bacterial meningitis. PMNs are often 100-10,000 while the lymphocyte count is <100. Protein is usually >1.0g/L but may be normal. Glucose is usually decreased but may be normal. PMNs may also occur in the early phase of viral meningitis, although lymphocytosis is more commonly seen. PMNs are usually <100, while lymphocytes are 10-1000. Protein may be 0.4-1g/L or may be normal. Glucose is usually normal. In tuberculous (TB) meningitis, the total WCC is usually < 500 x 106/L and lymphocytes predominate. Characteristically, the CSF glucose is low and CSF protein raised but normal values do not exclude TB meningitis.
|
|
Question 16 Which ONE of the following is the most common cause of bacterial meningitis in this age group? |
|---|
| Haemophilus influenza |
| Listeria monocytogenes |
| Group B streptococcus |
| Streptococcus pneumoniae |
| Neisseria meningitidis |
| Check answer |
ExplanationThe correct answer is: Neisseria meningitides. |
|
Question 17 Which ONE of the following treatments would you commence? |
|---|
| IV cefotaxime |
| IV ampicillin and gentamicin |
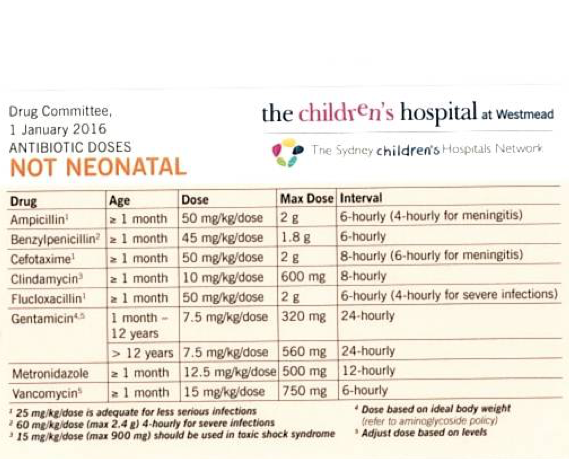
| IV cefotaxime and vancomycin |
| IV benzylpenicillin |
| IV flucloxacillin |
| Check answer |
ExplanationThree months – 15 years: Neisseria meningitidis (Meningococcus) is the most common organism. Haemophilus influenzae is now rare with Hib vaccination. Cefotaxime or ceftriaxone should be used empirically.
For more information, please seeNSW Health guideline: Infants and Children - Acute Management of Bacterial Meningitis |